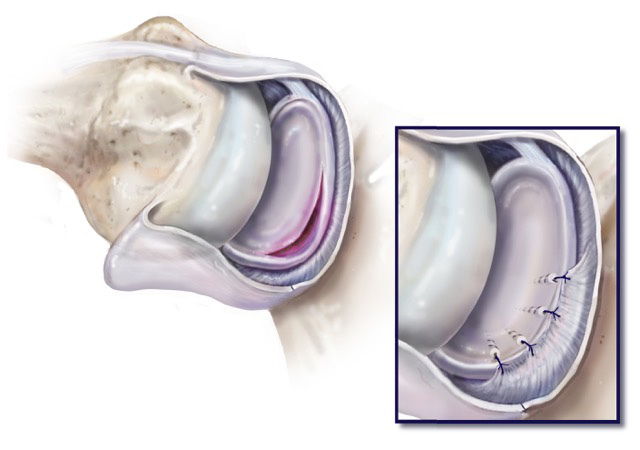
Arthroscopic Stabilization to Treat Shoulder Dislocations
A shoulder is considered "unstable" when it dislocates frequently or slips partially out of the joint. This is a condition known as subluxation. The shoulder is a 'ball and socket' type joint made up by the head of the upper arm bone (humerus) and the shoulder blade cavity (glenoid). In an unstable or 'loose' shoulder, the head of the humerus slips in and out of the shoulder glenoid (ball slips in and out of the socket), leading to a shoulder dislocation. This could be caused by injuries to a number of structures including the labrum, glenohumeral ligaments, joint capsule or rotator cuff.
Dislocated shoulder and shoulder instability is a very common and painful condition and results in limited motion and use of the arm because of the anxiety and worry that the dislocations can cause. Certain individuals are at very high risk of re-dislocating, and recurrent shoulder dislocations can cause significant disability. Furthermore, when a shoulder re-dislocates, there can be additional damage to the ligaments and the joint surfaces which may increase the risk of arthritis later in life. New arthroscopic, surgical techniques can be used to repair and stabilize shoulders after they dislocate. In some high risk individuals, arthroscopic stabilization surgery may be the best option, even after only a single dislocation. Arthroscopic repair minimizes pain, allows the surgery to be performed on an outpatient basis, and decreases the overall risk of complications.
If the injury is a more severe case and if minimally-invasive arthroscopic surgery will not repair the condition, then arthroscopic stabilization surgery will most likely need to be performed. Arthroscopic stabilization surgery (surgical shoulder stabilization) can be performed through an arthroscopic procedure involving the reattachment of loose or torn ligaments to the joint with the use of special implants called suture anchors. These anchors are used to relocate, hold in place and tighten injured joints. Once they are in place and the patient has begun a rehabilitation process, the sutures will eventually disintegrate.
For some patients, depending on their own individual shoulder instability, shoulder stabilization surgery can also help to repair shoulder tears of the biceps muscle tendon, bicep tendon injuries, rotator cuff injuries (tear), or help to tighten the shoulder capsule.
Shoulder arthroscopic stabilization surgery typically takes 1-2 hours. You will wake up in the Steadman Clinic's recovery room so that we can observe you for about an hour.
After Arthroscopic Stabilization Surgery
Here are some recommendations and what to expect once you arrive home after your arthroscopic shoulder stabilization surgery:
- After arthroscopic stabilization surgery, it is crucial that the arm remain immobile for a period of time. Therefore, we will put an immobilizer on our patients. This helps to decrease the chance for a new injury or injury to the repaired joint.
- Following shoulder stabilization surgery, we ask that you do not lift any heavy objects and that you get plenty of rest. There will be a 3-6 week period of complete shoulder immobility (no motion) while the joints heals. At the end of this period we will re-evaluate your shoulder.
- You will be instructed to do pendulum type exercises on your own. Pump your hand and move your wrist and elbow to keep the blood circulating and prevent stiffness.
- Our office will provide you with a special cold pack and we recommend using this to help control pain. Please protect your skin by using a small cloth or thin towel so that you can avoid burning or other skin irritations.
- Our office will prescribe pain medication to help you combat the pain you will be experiencing the first few days. Take this post-surgery pain medication, as prescribed, and use your cold pack to help with additional pain relief. In some cases, we will offer a pain pump to our patients. This is a small device that will be filled with numbing medicine that is attached to a catheter that we will place in the shoulder at the time of surgery. If you are using a pain pump, there will be a little button to push that will release the medication to help relieve the pain. This button can be pressed every 4-6 hours. This pump should be removed within 72 hours following shoulder surgery.
- In the hours following your arthroscopic surgery, please keep the post-operative dressing clean and dry. Unless it becomes wet or too tight because of swelling, leave the bandages in place for at least 2 days. REMOVE YOUR BANDAGES 2 days after your surgery. Cover your incisions with Band-Aids to keep from snagging the sutures on clothes. You may shower then, but try to keep the incisions dry for the first 10-14 days. Do not wet your incisions directly (bathing or swimming) until at least 2 weeks post-op.
- The sutures are absorbable and do not need to be removed.
- Be in the care of a responsible adult.
- Abstain from drinking alcoholic beverages and from smoking.
- You may eat a regular diet, if not nauseated. Drink plenty of non-alcoholic, non-caffeinated fluids.
- You will be required to visit our office for a post-operative visit within 10 days from shoulder stabilization arthroscopic surgery. We will evaluate the surgery site, discuss your progress, and put in place a rehabilitation program.
- Following this surgical procedure, please call our office if you are experiencing continued, intense shoulder pain, or if you have a temperature greater than 101 ºF. Please notify us if you experience numbness, a deep tingling, excessive drainage or excessive bleeding from the surgical site because they may represent a problem with the site.
Rehabilitation Following Shoulder Stabilization Surgery
Dr. Millett has specific guidelines for patients who have undergone arthroscopic surgery. These guidelines are broken down into various shoulder rehabilitation phases. Please refer to the Patient Resources section on this website to view a complete and printable version of the rehabilitation program. Depending on the extent of your injury and surgery, the rehab guidelines may vary. These are simply protocols for all patients who have had arthroscopic shoulder surgery.
To learn more about recurrent shoulder dislocations, or to determine if you are a candidate for arthroscopic stabilization surgery, please contact the orthopedic practice of Dr. Peter Millett.
Related Articles
What Treatment Options Exist for Shoulder Instability?
Does My Son Need Surgery for a Dislocated Shoulder?
I Dislocated my Shoulder and have Ongoing Shoulder Instability. Why?