An Overview of Shoulder Labral Tears and SLAP Tears
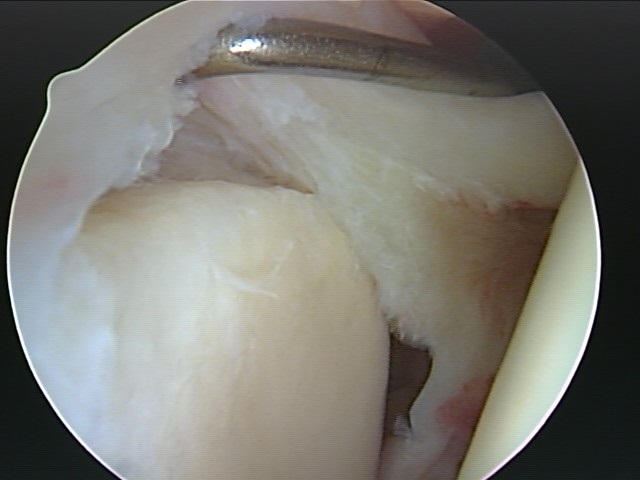
When the labrum, which is an important type of cartilage that surrounds the glenoid (the socket of the shoulder), is injured or torn, it is referred to as a shoulder labral tear. While the glenoid itself has a moderately flat surface, the labrum’s contour deepens the socket and gives the glenoid a concave shape, enhancing stability of the shoulder. The solid, firm, yet flexible fit of the humerus (the bone that extends from the shoulder to the elbow) within the glenoid permits the immense range motion that a healthy shoulder is able to exhibit.
A shoulder labral tear, which is quite common, is usually caused from falls when the arm is stretched out or from repetitive work or overhead sports activities (throwing, swimming, overhead lifting). A SLAP tear (Superior Labrum Anterior to Posterior) is a special type of tear in the labrum that occurs at the upper part of the labrum where the long head of the biceps tendon attaches to the glenoid. These types of injuries are particularly common in athletes who participate in overhead sports, such as tennis or baseball. An injury in this area can be extremely painful, and in severe cases can even cause bicep tendon tear or rupture.
When evaluating an individual who is suspected to have either a labral tear or a SLAP tear, it is important to determine if the labral tear is associated with any type of pre-existing instability to the shoulder. If instability is involved, then some type of shoulder stabilization procedure will need to take place first. X-rays will rule out any precursors or underlying problems that might exist such as an impingement or a fracture. If instability is not an issue or at the root of the problem, surgery can be directed to the labral tear itself.
Symptoms of Labral and SLAP Tears
The primary symptom of a shoulder labral tear is pain in the area of the injury—most commonly—at the back on top of the shoulder or deep inside the shoulder. The pain usually is intense and may be associated with mechanical symptoms such as clicking or catching. Shoulder stiffness can also be a sign of or associated with a labral tear. In throwers, there is a specific type of tightness of the posterior capsule called GIRD (glenohumeral internal rotation deficit) that may also need treatment. Labral tears involving the bicep tendon anchor (SLAP tears) can make using the biceps painful such that even performing small activities such as using a screwdriver can be painful or difficult.
Treatment of Shoulder Labral
and SLAP Tears
Non-Surgical
Much can be done to help individuals who suffer from labral or SLAP tears, and the first approach usually consists of icing, physical therapy exercises, anti-inflammatory medications and rest. Some shoulder labral tears can become asymptomatic (painless) and therefore may not need further treatment.
Surgical
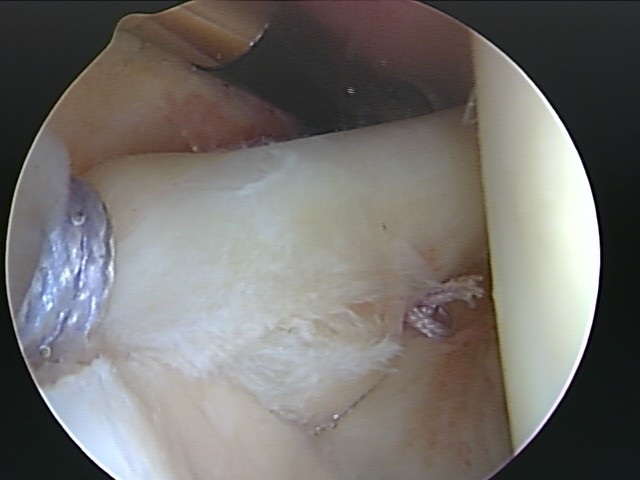
If the conservative approach to managing these tears is not effective, surgery may be required to repair or remove the torn part of the labrum. These are almost exclusively treated with arthroscopic surgery. Arthroscopic shoulder surgery is the standard treatment for most labral injuries, even those associated with instability, GIRD, rotator cuff tears, or biceps problems. The majority of these can be treated with simple debridement (removal of abnormal, damaged, or excess tissue) although sometimes detachment and repair of the biceps tendon (biceps tenodesis) is the preferred method of treatment. Dr Millett has performed several thousand of these procedures.
SLAP Repair Video
In certain painful and unstable SLAP tears, in which the bicep anchor is detached, the labrum will need to be repaired (labral or SLAP repair). This requires meticulous surgery so as not to create too much stiffness in the shoulder. Sutures and anchors are used to firmly re-attach the labrum to the bone of the glenoid. Rehabilitation after surgery is critical and most people can resume full activities by 3 months, although overhead sports may take a bit longer.
For additional resources on labral and SLAP tears, please contact the orthopedic office of Dr. Peter Millett.