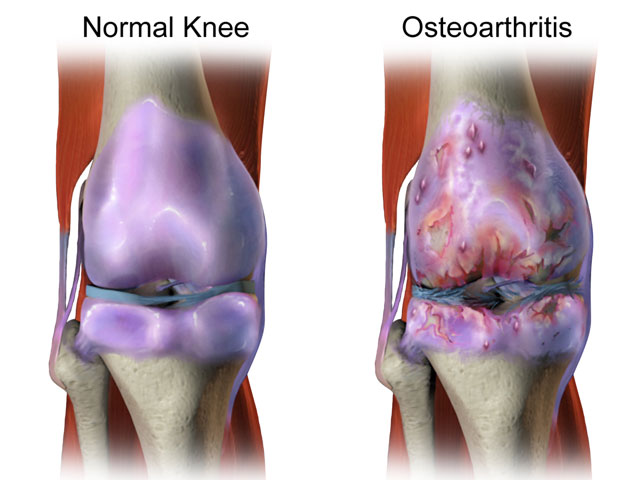
An Overview of Articular Cartilage Damage
Chondral knee injuries are the result of articular cartilage damage within the knee. Articular cartilage is a specific connective tissue covering joint surfaces that is important for smooth movement of the joint and allows the bones to move past each other without friction. Viewed by the naked eye, it has a glistening, white appearance. Microscopically, it is composed of water, collagen and a variety of matrix proteins and lipids.
Articular cartilage has no nerve supply and therefore does not cause immediate pain when it is injured. Once it is damaged, articular cartilage is unable to repair itself. Although symptoms related to articular cartilage damage may take years to develop, articular cartilage injury is very common.
Many factors play a role in chondral knee injuries, including the patient’s age when the degeneration starts, the patient’s activity level and weight, and the overall presence of ligament damage. Cartilage damage may be in place for years, but sometimes an individual is unaware because they remain asymptomatic. Years of wear-and-tear and bone-on-bone rubbing can cause symptoms to develop slowly over time as this cartilage damage progresses to osteoarthritis.
Chondral Knee Injuries Grading Scale
Chondral damage is graded from mild to severe, and all grades can have characteristics of osteoarthritis.
- Grade 0: Normal cartilage
- Grade I: In this early stage, cartilage starts to become soft and swells
- Grade II: This stage will present a partial-thickness defect with fibrillation (shredded appearance) or fissures (depressions) on the surface that do not reach the bone or exceed 1.5 cm in diameter.
- Grade III: This stage presents an increased amount of damage to the level of subchondral bone (bone right below the cartilage) in an area with a diameter more than 1.5 cm. Patients will often complain about noise as the knee bends and soreness or trouble standing from a squatted position.
- Grade IV: This phase will present an exposed subchondral bone—meaning, the cartilage may wear away completely. When the involved areas are large, pain usually becomes more severe, causing a limitation in activity.
Symptoms of Articular Cartilage Damage
The symptoms of a chondral injury resulting from articular cartilage damage will not present themselves as prominently as a torn ACL or meniscus tear. Similar to other arthritic conditions, the symptoms start mild and continue to progress as time goes on.
Symptoms with damaged articular knee cartilage, include:
- Intermittent swelling (often the only symptom)
- Pain associated with prolonged walking or stair climbing
- Buckling or giving way when full weight is placed on the knee
- Locking or catching
- The knee may make noise during motion
Diagnosing a chondral injury can be difficult. Many times, a swollen knee will show a normal exam. Imaging using an X-ray, MRI or via an arthroscopic examination can help determine if cartilage loss is occurring, thus leaving a decrease in space between the bone surfaces.
Treatment for Chondral Knee Injuries
Non-Surgical
Articular cartilage degeneration is often treated without surgery. Dr. Millett will recommend exercises to strengthen the muscles around the joint, supplements and possibly injections of regenerative medicine, such as PRP (platelet rich plasma) or hyaluronic acid, to improve joint lubrication and reduce friction. There are medications that can be prescribed to help treat symptoms associated with chondral injuries. However, since new growth of cartilage is challenging, most medications presently will not cure the condition. Medications and other treatments however can allow patients to live pain-free and remain active.
Surgical
Over the past decade, there have been big strides and exciting advancements in the surgical treatment of articular cartilage defects. The most commonly performed procedures for treating chondral defects include chondroplasty (cartilage removal), microfracture (holes made in bones that release stem cells from the marrow), and OATS, or OsteoArticular Transfer – this can be done by taking a piece of bone and cartilage from elsewhere in one’s knee or from a cadaver knee and then transplanting it into the defective area.
Chondroplasty – Shaving or Debridement
This arthroscopic surgery technique uses special arthroscopic instruments to smooth the shredded or frayed articular cartilage. Ideally, this treatment will decrease friction and irritation, reducing the symptoms of swelling, noise, and pain.
Microfracture
This arthroscopic technique encourages the growth of new cartilage into the defect. This is a well-accepted technique that is a common procedure for patients with damage through the full thickness of articular cartilage (all the way to the bone).
OATS
OATS, osteochondral autograft transfer system, is a technique that involves replacing damaged joint cartilage (in high weight bearing areas) with healthy cartilage and bone (from lower weight bearing areas). This is an arthroscopic or open procedure done using either one’s own healthy tissue or tissue transplanted from a cadaver. Small holes are drilled into the damaged cartilage area. Then, bone and cartilage grafts are inserted into the defective area to re-surface the damaged cartilage. It is highly effective.