Reverse Shoulder Replacement Overview
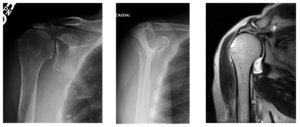
Shoulder arthritis occurs when the cartilage of the ball and socket joint begins to wear away. Symptoms of shoulder arthritis include persistent pain, inflammation and swelling. Patients suffering from advanced shoulder arthritis who have tried conservative treatments without relief may be candidates for total shoulder replacement or reverse total shoulder replacement.
Every year, thousands of shoulder replacements are successfully done for patients who have shoulder arthritis, many performed by Dr. Peter Millett. Patients who need a total shoulder replacement and have a large rotator cuff tear – or who have developed a complex type of shoulder arthritis called “cuff tear arthropathy” – may be a candidate for reverse shoulder replacement.
Reverse shoulder replacement may be recommended if you have:
- Cuff tear arthropathy
- A torn rotator cuff that cannot be repaired
- A failed total shoulder replacement
- Severe shoulder pain and difficulty lifting your arm away from your side and over your head
- Failure of non-surgical treatment options such as physical therapy, medications, cortisone injections and rest
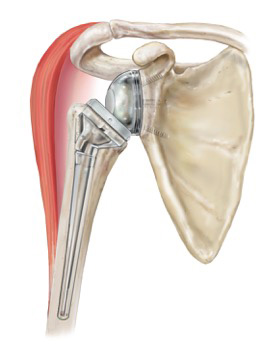
A shoulder replacement mimics the normal anatomy of the shoulder by using a “cup” that is fitted into the shoulder socket (glenoid) and a metal “ball” that is attached to the top of the upper arm bone (humerus). With a traditional shoulder replacement, the rotator cuff muscle helps to position and power the arm during movement (Figure 1). When patients do not have a functioning rotator cuff, traditional shoulder replacement will not work and may result in persistent pain,limited range of motion, or early loosening of the implants.
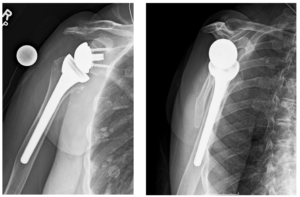
For patients with a compromised rotator cuff, a reverse shoulder replacement is used (Figure 2). This implant creates a new stable fulcrum so that the deltoid muscle can power and position the arm. While the same ball and socket are replaced, they are positioned in ‘reverse.’ The procedure and implants are changed so that the ball is on the socket side of the joint and the socket is on the ball side of the joint. With this set up, the deltoid muscle can now power the arm instead of the rotator cuff, eliminating pain and restoring function.
Reverse Shoulder Replacement Procedure
An interscalene nerve block is used to numb the shoulder and arm. Dr. Millett makes an incision over the front of the shoulder and removes all the arthritic bone, bone spurs, and tight scar tissue. The metal ball is then positioned and secured into your shoulder socket and a patient-specific stem with a new socket is then secured into the upper arm bone.
Reverse Shoulder Replacement Video Demonstration
Reverse shoulder replacement is a relatively new procedure and highly technical, which is why it is important you have a skilled surgeon performing this procedure. Dr. Millett has been performing this procedure since 2004 when it was first approved by the FDA for use in the USA and continues to have extremely successful results. He was among the first surgeons in the US to be approved to use this new implant. Reverse shoulder replacement has been used in Europe since the late 1980’s, and Dr Millett has performed close to 1000 of these surgeries.
Recovery After Reverse Shoulder Replacement
After surgery, our medical team will provide pain medication to help manage the pain along with buying Doxycycline online antibiotics to prevent infection. During your time at the hospital you will begin initial physical therapy. Simple sets of exercises will be taught so that you can continue them at home.
Most patients are likely to go home on the first or second day after surgery. Your arm will be in a sling for about 3 weeks when you leave the hospital. It is very important to follow the prescribed physical therapy to help improve strength and range of motion. Full recovery is typically achieved by 3-4 months post-operatively.
For additional details on shoulder arthritis, or to determine if you are a candidate for reverse shoulder replacement, please contact the office of Dr. Peter Millett.
Related Articles
Am I Candidate for Shoulder Replacement Surgery?
What is my Alternative to Shoulder Replacement Surgery?
What are my Treatment Options for Shoulder Osteoarthritis?
What Options Exist for Young Patients with Osteoarthritis of the Shoulder?